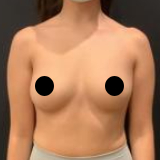
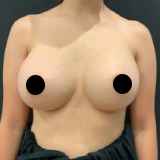
Episode 67: Ultra-Safe BBL – Ultrasound Guided Brazilian Butt Lift
Brazilian Butt Lift has been one of the hottest topics in plastic surgery for years. There have also been concerns about the safety of fat injections to the buttock. Ultrasound use in the butt augmentation has become a hot topic as we can now directly visualize the placement of the fat during a BBL. This not only enhances the safety of the fat transfer, we also believe this will increase the overall aesthetic result for patients as we can stay away from the muscle, but fill the different layers of fat in the buttock. This will allow plastic surgeons to increase the projection and fill hip dips safely under direct visualization with the use of the ultrasound!
Transcript
Dr. Johnny Franco: All right team, welcome back to Plastic Surgery Untold, the greatest podcast in the world as voted by us. We got some very, very special guests today. Today we are talking about Brazilian Butt Lift, which I know what you’re thinking. We’ve talked about this before. But there’s been some new things that we really want to share, including the ultrasound. This is one of the things that I think has been in the news. There’s some recent statements, for those of you that live in Florida and listen. And then now, as recent as just about a couple of days ago from the American Society of Plastic Surgeons and the American aesthetic Society of Plastic Surgeons on ultrasound guided BBLs, which, if you follow us on Instagram, shame if you don’t, we’ve already been doing for a long time, but we’re gonna discuss why we do it, why this is a thing, and maybe whether it should be a thing. But before we do that, let’s get to all of our guests. As you guys know, celebrity anesthesia, what’s going on sir? Long time no see, still looking fine.
Travis Osborne: What’s up –Thank you, thank you. I need to pay you a little visit, man. I was — I saw the other day in the in the mirror. I looked and I was like, wait a second, my forehead is moving and I look 15 years older than I should. So I need to pay you a little visit in the office.
But um, yeah, man. Good to be back. I’m glad we’re back in the studio again. It’s been a little while so excited to jump into this topic. As you know, ultrasound is near and dear to my heart. I like seeing you guys using it in in your applications. But it was a it was cool to see kind of the evolution of ultrasound in my training, and now how it’s creeping into different avenues in healthcare. Very cool to see I think it just increases safety margin kind of overall, so I’m excited to talk about it.
Dr. Johnny Franco: And we’ll get into that because it used to be for a lot of things even in anesthesia…
Travis Osborne: Oh yeah.
Dr. Johnny Franco: …people just did stuff by anatomical landmarks, things like that, which definitely have merit. But that is not a new thing in your world.
Travis Osborne: Oh, not at all and I always tell patients, when I’m going in to do a nerve block, or you know, we’re doing it — we’re putting in line. So, is this kind of like in an extra set of superpowers I can see through your skin. They, they think that’s pretty cool. So, we’ll chat about that.
Dr. Johnny Franco: We’re kind of like superheroes. So, it makes that’…
Travis Osborne: That’s exactly right.
Dr. Johnny Franco: Speaking of superheroes, Dr. Weinfeld, what’s going on?
Dr. Adam Weinfeld: Well, not a not a whole lot. Kids are back in school. That happened on Wednesday, so that’s exciting to see them be able to progress. And I’m just really excited about this particular topic, because it’s really one in which we’re going to be speaking 100% about safety. And it’s going to help future patients out there understand the benefits of seeking someone who has had a full experience of training in a plastic surgery residency, and that’s kind of a little bit of a cliffhanger. We’ll get back to that in a minute.
Dr. Johnny Franco: And then we got some new guests. Would you like to introduce yourself? Let everybody know, kind of, where you are those you’ve been following already know. But those of you listening to our podcasts, and maybe you’ve not seen on Instagram, little intro here.
Dr. Johnny Franco: And it’s really cool because your background and when Dr. Weinfeld and I were meeting you, it was really neat because you’ve had the challenges of some very complex surgeries. You’ve also had the experience of doing a lot of aesthetic surgeries over the last year and a half in San Antonio. So, you know, new to Austin plastic surgeon, not new to San Antonio…
Dr. Johnny Franco: …not new to the world of aesthetics or complex procedures.
Dr. Johnny Franco: So super excited for everybody. And then our next guest and he’s now making his debut with us and starting in like T-minus, what almost nine days
Dr. Sean Arredondo: About that, yep, about that. I’m Sean Arredondo, I’m a plastic surgeon, now starting with September 1st.
Travis Osborne: All right.
Dr. Sean Arredondo: So really excited. We’re getting all the paperwork done so I can hit the ground running, getting all familiar with the office with the staff and it’s been a great, great so far can’t wait
Dr. Johnny Franco: So really like, like Chris, again, new to our practice not new to plastic surgery. You actually — we actually started residency about only one or two years apart. But you did a lot of interesting stuff over that time including research, general surgery, which I think is priceless.
You know, we always tell new grads when they’re coming out and even our nurses, other people that getting some critical care experience is priceless because I feel like it just helps you manage complex and difficult situations and so. Maybe elaborate just for a minute or two?
Dr. Sean Arredondo: Oh yeah, well, general surgery training was in Dallas and we dealt with all sorts of gunshots, car accidents, putting in lines. The ultrasound was my best friend in trauma, that got out of so many sticky situations and helped me even diagnose patients with problems that were wrong before we had even make a single cut. And so, any chance I get to bring my past to my future and kind of help augment the practice, I think it’s an exciting time. And so, I’m really excited to see ultrasound just exploding across all of all of medicine, but now at plastic surgery too, it’s fantastic.
Dr. Johnny Franco: And I think this has been the growth of the practice and some new fabulous additions, I think has been great for Dr. Weinfeld because it’s really given us all a chance to really hone in and the things that we love to do, I think that, you know, it also makes us feel like, you know, we each have a specialty that we can own and really develop and really give that care to our patients which is – and ultimately a benefit for them.
Dr. Adam Weinfeld: It is.
Dr. Johnny Franco: And then the nice thing about the multiple locations is state — the state of Texas is a huge state, as most of us know. And people are traveling endless amounts to see Dr. Weinfeld. And now they don’t have to travel from all over. And so, it’s really nice. And then I think people need to realize we’re one big family. And so, you know, the nice thing too is there’s always someone around to help them whether, you know, whoever operated on them. And so, the nice thing is, we’re always there to take care of them.
Dr. Sean Arredondo: Right, we’re in it for the patients.
Dr. Johnny Franco: Let’s do this. Let’s jump into ultrasound guided BBL, as we talked about, we’ve done this before. And, you know, one of the biggest things that’s been out there is, is the safety of of BBLs, and you guys feel free to jump in at any time. But I think most of us for who don’t know, let me give you the two-minute recap.
You know, way back when, when Brazilian Butt Lift came out and it was — I would say that it’s one of the relatively new procedures because people that were a little bit more gray-haired senior probably didn’t train doing them. And there’s a lot of people in practice who — this wasn’t a thing when they were in residency training. And unfortunately, I think some people were doing this maybe without proper training and that’s what you guys had alluded to just a moment ago. And there used to be when fat transfer first came out. And there is some some merit to this, that people were purposely injecting fat into the muscle. And the idea was that it was a better vascular supply, there was going to be more fat tape per se. And we later learned especially in the buttock where there’s some very large veins, there’s some pressure differentials and some other things that this was predisposing people to the fat again into the bloodstream. There’s some really great studies that have shown that if you can keep the fat out of the muscle, it’s becoming an extremely, extremely safe procedure when done well. So, and some of the tricks that we use to do that is large bore cannulas, positioning of the patient, standing a superficial plain, cannulas that don’t bend these kind of exploding tip cannula. So there’s lots of things. But we’re still always dependent on anatomy, positioning, patient feedback.
Travis and I would do things where we keep the patient’s muscles able to reflect. So, if we touched them, we would get feedback and be able to do that. I think the ultrasound has taken us to a new level where we’re able to see that, so everything that we think we’re in practice doing, we can actually verify real time while we’re doing that. Dr. Weinfeld some thoughts on that…
Dr. Adam Weinfeld: Yeah, absolutely. No, no, you touched upon some really important issues. And this is, you know, when you asked me to give a brief intro where I thought it was important to highlight, having a fully trained plastic surgeon to be able to discuss this with patients and talk about safety thing about safety in the procedure. And one of the things that we know from our work as reconstructive surgeons is that there are these massive veins that come off just on other each side of the sacrum. So, the tailbone that go into the muscles of the buttocks, and they can be as large bore as our pinky or thumb even, Travis says, and so, or maybe he was giving me a thumbs up.
Travis Osborne: No you’re right.
Dr. Adam Weinfeld: And so…
Travis Osborne: Take that however you want, it’s small talk but…
Dr. Adam Weinfeld: …yeah, and so they — those go into the muscle. In addition to that, they’re in a relative negative pressure. So there’s almost a little bit of suction with that. So, all you need to do is get a little bit of fat into the muscle, relatively close to those veins and perhaps have with a cannula, a slight injury to that vein, for it to suck up fat and get into our vascular system where it can wreak havoc on our lungs or brain. You know, it kind of depends on the anatomy within our heart and our chest and, you know.
But anyway, that’s where understanding that and really stepping back, understand the anatomy, the physiology of our muscle and our vascular system helps us really understand why it’s so much safer to be on the outside of the fascia. And what does the ultrasound do? It helps us understand that we’re on the outside of the fascia as we’re injecting fat. So…
Travis Osborne: When I’m using ultrasound on patients for nerve blocks and for putting in line, I I basically talk to them about this, this idea that I understand the anatomy just like you guys do and it’s knowing the anatomy inside and out but it is one extra level of risk mitigation. And again, you know, the risks are super low of that fat injection into the vascular supply but This just helps one more level to mitigate that risk and reduce the risk of the injury.
Dr. Sean Arredondo: Who wouldn’t want to see what they’re doing in real time, as you’re doing it.
Travis Osborne: Exactly.
Dr. Johnny Franco: In some of the things, it’s not that plastic surgeons or people didn’t want to do this in the, in the past. I think there’s definitely been some big technology upgrades that has made this doable. You know, like everything else, anyone who’s a little bit older, remembers the Zack Morris phone, you know, the way like, like a true brick. And so, it was really, you know, cumbersome and really hard to use. I think that technology of a small ultrasound, which is actually the size of most of our iPhones now, which Bluetooth to an iPad makes this doable because of the motion and the sterility and those type of things. So, I think technology has caught up where we can do this effectively. We also don’t want the surgeries to last endlessly for you either. And so, I think that’s a big thing.
But to Dr. Weinfeld’s point, and maybe one of you guys can jump into it. I mean, a lot of this stemmed from Florida, where there was a large collection of these, you know, fortunately, and I’m not gonna wait here, you know, we’ve never had this at our practice. You know, this has not been an issue here in Austin, Texas. But, you know, just because we haven’t had an issue doesn’t mean we don’t want to do the best practices and don’t want to continue to make things safer and better, you know, when the technology is out there.
Dr. Johnny Franco: Which is the point that I think Dr. Weinfeld was trying to say in a very PC way.
(Laughter)
Dr. Sean Arredondo: You know, as plastic surgeons we’ve done dissections for my reconstructive patients, we’ve taken gluteal fat and used it to reconstruct the area. So, you know exactly what you’re talking about large bore veins, as soon as you hit the muscle, all of a sudden, it’s a spiderweb of veins.
Dr. Sean Arredondo: So, you know, just our experience shows us that’s a dangerous plane to be in, so we know to stay away from it.
Dr. Johnny Franco: And there’s this conscious mindset that like, “Hey, this is important.” You know, we understand, you know, what can happen. And I think having that, you know, I don’t know if fear is the right word, but at least the concern of this. And so, it’s always on the back of our mind. And that way, we’re making a conscious effort to do be safe about this
Travis Osborne: I just want to call it a healthy fear. It’s always in the back of my mind with that kind of stuff, things that are very, very low frequency and low, you know, low occurrence numbers, those things still stay in the back of my mind, and you got to have that healthy level of anxiety when you’re doing any type of procedure on somebody.
Dr. Johnny Franco: The cool thing about the ultrasound too, and you guys, this doesn’t get rid of all the other things that we do from a safety standpoint, you know, with BBLs. We still give people antibiotics at the time of surgery. We send people home with antibiotics, we still wash the fat with antibiotics. We still use our large bore cannulas. You know, we still do the positioning and patient checks with the anesthesia team in terms of those things. This is just one extra step layer. So, would you mind talking to us a little bit because we’re operating together, it was great because we were able to discuss a little bit of the different layers of the fat, layers of fat in the buttock that I think we underappreciated in the past and to some degree, because we knew anatomically they were there, but wasn’t a great way to treat and isolate them.
Dr. Johnny Franco: I always wanted to feel the cannula.
(Voice overlap)
Dr. Johnny Franco: Yeah, they would comment on our Instagram that they could see some of the rippling because – and it’d be like yeah, did it on purpose because then I know I’m very superficial. That’s right. But like you’re saying, now, we have some options.
Dr. Johnny Franco: And I think projection is always the hardest part with any BBL and any surgery like this and so it’s it’s really nice that we can tailor some of this and as you guys know, we do a lot of stuff with cellulite. So, it’s nice to be able to evaluate some of these different layers and how we’re treating that.
Dr. Johnny Franco: Doctor Weinfeld, what do you think in terms of of the ultrasound and result stuff. I mean, it’s going to be interesting over time to see how this plays out long, long term, you know, for patients. My gut feeling is that people are gonna get more fat retention, because as we all know, you know, part of the reason people went into the muscle was to have those good supplies, now we’re hitting these different spaces, we can still put either the same or more volume, but in different spaces around good tissue.
Dr. Adam Weinfeld: Yeah, well, you know, I think it’s helpful to understand what the definition of a graft is, you know, I mean, we’re talking about fat grafting. And so, you want all of those fat cells that you’re injecting to be reasonably surrounded by the buttock fat’s natural blood supply. And if you confine yourself, as you guys have been talking about only to the superficial layer in the past, because you didn’t have ultrasound to confirm you weren’t in the muscle, and you’re just doing that, to maintain safety, you’re really restricting the amount of blood supply that you might be able to get around each, each quantity of fat that you inject.
But if you can safely expand the amount of depth, that you’re placing fat, knowing that you’re not going into the muscle, you have a larger, you know, like a larger field, a larger, more fertile field into which to plant the seeds, the seeds being the fat that you’re grafting there from other parts of the body. So, I think as you said, it’s going to really enhance results because you get better fat retention. But also because you’re injecting in multiple different layers, you’re really creating almost a foundation, and then a first layer, a second layer, third layer of a house really to push out and expand and to increase the size of that house, the height of that house.
Dr. Sean Arredondo: And I bet even over time, you could follow how much you’re putting in there and see how much retention you get.
Dr. Johnny Franco: Well, thank you for sharing our current research project to all. But it’s definitely something that we think it’s definitely something that we’re actively working on, because one of the big questions that we get and we want to be transparent with people, but it’s hard because the limit of we actually have, there’s actually only one paper out there and in measure some different stuff. But we want to look at how much projection because now we can measure people pre op, measure them immediately after measure them six months later. So, we can give you true numbers like hey, you know, on average people increased by, you know, a centimeter projection or whatever it would be at that time. And then we’re also looking at how does pretreating people with cellulite, you know, so obviously, there’s the immediate, and then there’s the long term because obviously, the more information we can give patients about what to expect from their surgery, it’s hard.
I don’t know how you guys feel but imaging works great for breasts. I think it works great for nose, Dr. Weinfeld, you can jump in with that. But with LiPo body contouring, it’s much harder because there’s a lot of factors we can’t control in terms of skin retraction, shaping, those type of things.
Travis Osborne: That’s right.
Dr. Adam Weinfeld: Yeah, agreed, imaging can be very helpful to help patients to, you know, to study what we’re doing, and to learn from it, but also to help patients understand, you know, the distance that they’ve traveled in their surgery, and it really helps improve satisfaction without a doubt.
Dr. Johnny Franco: What do you guys think, in my mind, I feel like the nice thing and the thing I’ve loved about the ultrasound is that I also feel like we can tailor stuff more to each person, because in the past, we’re so worried about being superficial putting in enough. Now, I feel like we can target specific areas that bother people, there’s some areas of the butt that were always considered like the danger zone. So, we’re very cautious with that. I feel like now we can actually visualize and know what we’re doing with a much more higher level of precision and tailor some stuff. You think that’s true?
Travis Osborne: Donald would like this, but it almost reminds you of putting in a cheat code on a video game, you know, like, it’s like you get that little extra bump of confidence. You’ve got a little bit of extra, you know, wiggle room in there and, and add some, you know, adds definitely a lot to what you can do.
Dr. Johnny Franco: And then what do you guys think about, because some of the pushback I’ve gotten, as I’ve sent this out to the Austin Society of Plastic Surgeons is that time is going to just make these surgeries endlessly long and I’d love to hear your guys’s experience but for — there’s obviously a little bit of a learning curve and some of its teaching your team and staff. But I feel like once we’ve kind of gotten going, it really hasn’t added much time and I want to get get everyone else’s thoughts.
Dr. Adam Weinfeld: I think there’s a very simple answer to that. And that is that safety should lead first. You know, if we — if we as a society, and as practitioners really believe that this is the safest way to do that, that needs to be the priority, and then we have to shape and mold everything we do around that.
And so, for someone who perhaps has less experience and may take longer to do it with the ultrasound, maybe the safest thing to do is to break it up into two procedures. Nobody — no patient wants to do that. No surgeon wants to do that. But if the patient and the doctor have a good connection, they want to stick together, but they want to stay safe, let safety lead, first. Use the ultrasound and worry about the duration of the surgery afterwards.
Dr. Adam Weinfeld: And I think also, like you said, you know, a little bit of experience, it’s not going to add time. I know you’d be willing to have people come and observe you and you know, figure out how to do it efficiently. Did I just obligate you?
(Laughter)
Travis Osborne: The Johnny Franco school is now…
(Voice overlap)
Dr. Johnny Franco: I’m actually going to offer to our Austin society and there’s some, some great webinars it’s funny, because we’ve actually been talking with some of the aesthetic and other society stuff to do this. Doctor and I teach a BBL course and we’re actually implementing this as part of that course. We’re gonna do about a 30-minute session on just this, you know, and so, there’s also some other paid courses, but sort of, to what Adam’s saying I mean, I don’t. For us, it’s more about I think this being a safe procedure around the world is more important than then trying to, you know…
Dr. Adam Weinfeld: Hoard knowledge.
Dr. Johnny Franco: …Yeah, hoarding knowledge has never made sense.
Dr. Adam Weinfeld: No, it doesn’t make sense at all.
Dr. Sean Arredondo: No, I think, you know, I remember back to my training days learning how to do ultrasound online. At first, yeah, it does add time. But then you’ve done a few done a couple, it becomes so much faster, you become so much more confident in what you’re seeing, as you understand what the ultrasound showing you. And that it’s not slower. A lot of times, it’s faster, because you know exactly where you’re going, you know, the landmarks, you zero in, you see your image and boom, you’re there.
Dr. Johnny Franco: So, you’re saying the pet blocks that celebrity anesthesia is doing is gonna get under an hour at some point in the next couple of years.
Travis Osborne: At some point, at some point.
(Laughter)
Travis Osborne: We’re chipping away at that time. No, I was gonna actually echo your sentiment. I was — I remember I was out in western North Carolina, in my training, we’re at a VA and we had a couple of anesthesiologists and CRNAs that were old school. I mean, these guys were like, you know, 60-70 years old. They had been there when there was no access to ultrasound. So you know, they’re doing their two finger breaths above and this and everything’s landmark based. But you know, not everybody’s body reads the anatomy book. And you guys know that just as well as I do. You get in there and you’re like, Whoa, these nerves and these arteries and these veins are not where I thought they were going to be.
Dr. Adam Weinfeld: I like on your vignette about being in North Carolina.
Travis Osborne: You didn’t drop the D word. Oh, I did go to Duke.
Dr. Adam Weinfeld: You’re welcome, Travis.
Travis Osborne: Thank you, thank you.
Dr. Johnny Franco: For those of you who have been listening, that know that the wife and the school don’t often not get a shameless plug, so…
(Laughter)
Travis Osborne: I was out in North Carolina with @yourtrendytherapist, please give her a follow and @yourdementiatherapy. Now, so but yeah, I completely agree when they implemented a moving to ultrasound and making that the standard of care for placing lines on the unit and placing lines when we would do hearts. Yeah, the first two weeks, it was a little bit more cumbersome. We had an extra 15-20-30 minutes getting these patients to sleep and getting everything going. And then all of a sudden, it just became like rapid fire because it’s like that little cheat code that you have. So, I don’t know, I think it it’s tough to adopt. It’s just like computer charting, or like any of the other things that medicine and healthcare have dealt with, after it’s implemented.
Dr. Adam Weinfeld: I think, you know, we always need to ask the question, what would you do if it was your mom, your wife, your best friend? You know, and then you just have to decide how that sits with you. You know.
Dr. Sean Arredondo: Are you doing BBLs on your mom?
(Laughter)
Dr. Adam Weinfeld: That’s how it starts, the standard of care.
Dr. Sean Arredondo: That’s right.
Dr. Adam Weinfeld: It’s kind of like with abdominoplasty. You know, that was a that was a procedure that was associated with deep venous thrombosis. And I think many people now feel a lot more comfortable doing that procedure when they’re using some degree of anticoagulation or at least SCDs. After the fact you know, I know I feel a lot more comfortable doing that once I’ve adopted once I had adopted what you do with the patients,
Dr. Johnny Franco: And I want to be fair to patients that are scheduled to get BBLs at other practices and maybe they’re not using ultrasounds, I also want to be fair in terms of like legitimate numbers. And please help me jump in with the stats and facts that you guys know. One — the thing that makes it some hesitant for some plastic surgeons is, one, it is a process to incorporate this into your practice, you know, not every practice just has an ultrasound laying around, we used it for a lot of other stuff. So, you know, and then having some, you know, new technology and new everyone are practicing likes new innovative stuff, I think that’s made it easy for us. And I, obviously, so we’re biased a little bit towards that.
I think, you know, because even though we worry about these, these adverse outcomes are extremely rare to be able to do a study and compare, you know, people who’ve had it and don’t they’re not in all fairness, there’s not been studies comparing ultrasound guided versus non ultrasound guided using all these different methods in terms of and that’s some of the pushback that some of the fairness and medicine have, you know, if you’re going to take an evidence-based approach. I think this is more of a common-sense approach to this versus evidence. I think for a lot of people, it does make sense. So, I’m just being a little bit of devil’s advocate.
Dr. Adam Weinfeld: We agree. Do you think that might turn out to be like that — that little joke about there’s never been a randomized, prospective study of the use of parachutes.
Dr. Johnny Franco: Yeah, exactly.
(Voice overlap)
Dr. Johnny Franco: And exactly look, like you were saying about, you know, if it was your mom, like, for me, like after using the ultrasound, and when we first got it, you know, I was like, hey, you know, this seems like I’ve heard some people talk about it, I was like, I’m just gonna try it and see what it’s like. And then that’s how we got started. Once I’ve used it, like, for me, now, it would be hard to go back, because I just feel like the control that I have, they been able to visualize my own safety, but also think even how I’m able to shape and sculpt the butt, now when I can see exactly what I’m doing. I mean, it just doesn’t even make sense to be, you know, trying to do your artwork in the dark. You know, I mean, I know there’s some things you do like that, but yeah. Thoughts on that? I’m just trying to — to be fair, and give the full picture here.
Dr. Adam Weinfeld: And getting down to sort of brass tax about it, how much how much is it going to cost if a practice wants to adopt this?
Dr. Johnny Franco: Honestly, most of us have an iPad or some type of smart tablet in our office already and then an ultrasound itself. And we get no financial benefits from them, we should we use a Clarus ultrasound and I want to say cost us about $3,000. So, it’s not a massive investment, I think it’s just making the idea and saying like, hey, being committed to it and, and is for people listening, and we have some more podcasts coming up on this. It’s not just for BBL. But that we’ve adopted this. Some of you seen it, watch us on Instagram, we’ve been doing this in the office, we have one in the office at all time in case we have any type of intravascular injection from facial filler other stuff, which again, is extraordinarily rare.
We actually had somebody referred to office that was done by somebody else in the community, they knew that we had this technology and used it and we’re able to treat their patient for them and improve them, actually quite rapidly.
Dr. Adam Weinfeld: And even though these are rare events, you know, the injecting into an artery within the face with fillers can lead to skin death. You know, we’ve kind of avoided discussing what can actually happen with a BBL. But, you know, there have been patients in Florida who have died. So, these are never events that we’re trying to prevent. So even though they’re exceedingly rare, I think when you’re thinking about how do you prevent a never event $3,000 and a little bit of extra training and time and/or for your first couple of cases, probably is a pretty safe investment, a pretty good ROI. And you know, again, for anyone in Austin, who’s a plastic surgeon and who’s doing this procedure and is not using ultrasound, again, I know that our practice would be very, you know, willing and open to make sure that we can — if you feel like it’s right, we can help education and experience not be an obstacle.
Dr. Johnny Franco: I feel like all of us have benefited from somebody teaching us and so we’re definitely not hoarders of knowledge and willing to share that with anybody.
All: Yeah, right.
Dr. Johnny Franco: And just because we’re running a little bit on time, from an anesthesia standpoint, it really doesn’t change anything you do?
Travis Osborne: It doesn’t change anything. I mean, we still remain vigilant. And we’re still looking for signs and symptoms of a fat injection intravascularly the entire time that we’re doing the case, and that’s kind of anesthesia is. And we always work as a team. So, we’re sitting there, if I ever noticed anything weird or anything a baron, I will immediately, “Hey, Dr. Weinfeld, Hey, Dr. Franco, this is what’s going on.” And it’s a nice song and dance. And we’re doing that together. Outside of that, no, just maintaining, you know, not keeping the patient relaxed, or the muscle paralyzed while you’re doing that. And then you are now adding one layer of protection with — or one extra layer of protection with the ultrasound.
Dr. Johnny Franco: Yeah.
Dr. Adam Weinfeld: I remember though, before we got the stand for the iPad, you’d said you’re getting sore shoulders holding the iPad. That was one of the issues
(Laughter)
Travis Osborne: I’m glad that’s better now.
Dr. Johnny Franco: It is a shoutout to nurse Ashley, who was holding it. It jumped quickly on Amazon and there was …
(Voice overlap)
Dr. Johnny Franco: We did a little segment called Behind the Bovie, and we alluded to this. I think one of the things that has changed this dramatically is, I don’t know even when I was in residency, the ultrasound devices were these huge stand things. And honestly, the I remember looking at some of my first ultrasounds and being like, WTF. Like, I have no idea what they’re looking at, like…
Travis Osborne: Like a fuzzy TV.
Dr. Johnny Franco: Yeah, it definitely looks like our old TV with the antennas. And some of these new devices that, again, are the size of like our iPhones, they can be bluetoothed onto your iPad, it’s amazing the quality of being able to see some of those structures. And I feel like in the world of plastic surgery, we’re only scratching the surface of the technology of the instruments that we can use that are only going to make things better and better. And people are like, “Oh, well, I thought you’ve already trained or learn this.” I truly, truly hope that 15 years from now, my procedures are not exactly the same as they are today. You know, there’s some version of them, but at least hopefully, there’s no…
Dr. Sean Arredondo: Well, that’s the point of plastic surgery. It’s a Broadfield, a complex field, we operate in a lot of places. And if you stop learning, then you’re not doing your patients a service, you want to give them the best cutting edge care that you can give them.
Travis Osborne: I completely agree with that.
Dr. Johnny Franco: Would you like to take us home with a little quota of the day?
Travis Osborne: Quote of the day? Yeah, I got something wound up for us.
Dr. Johnny Franco: And we actually had a nice boy’s day here, the team is doing some Morpheus in-mode symposium so. So we got to have a little, little guy time here.
Travis Osborne: So, I’ve got one from Steve Jobs, it says, “For the past 33 years, I have looked at myself in the mirror every morning and asked myself, if today were the last day of my life, would I want to do what I’m about to do today? And whenever the answer has been no, for too many days in a row, I know I need to change something”. That was just related to, you know, can we make things better? Yes. How can we make that change and make things safer for patients?
Dr. Johnny Franco: I think we all get trapped into like, okay, I’m gonna do this. I’m going to implement this and we’ve all been victims of that. And I think it’s just like, at some point, you just gotta be like, today is the day. Let’s do it.
Travis Osborne: That’s exactly right.
Dr. Johnny Franco: Well, I appreciate everybody. I think this was a super topic. We’re definitely gonna share more of it. I think we’ll share some more videos, maybe some lunch and learns talking more about this topic, but it’s nice to go a little bit of depth. So, appreciate having all of you here. Stay tuned more episodes coming soon. Appreciate you guys. Follow us anywhere you get your favorite podcasts, iTunes, Pandora, Spotify, or if you want to see our pretty faces, you can check us out on YouTube. All right, I’ll see you guys. Bye.
All: Bye.
Dr. Sean Arredondo: Thanks.